The Future of Medical Exercise: Why Functional Assessment Scales Are the Ultimate Game Changer
Get the podcast here
For the last thirty plus years I have learned a simple but uncomfortable truth about medical exercise.
Most fitness professionals measure the wrong things.
They measure strength, flexibility, and endurance in isolation. They celebrate improvements in numbers that mean something inside the fitness industry but mean very little inside the healthcare system.
A physician does not care that your client improved their squat by 25 pounds.
A physician cares whether that person can safely climb stairs, walk without falling, return to work, or maintain independence.
This is the fundamental shift that is now occurring in the evolution of medical exercise training.
The future of the profession will be built not on exercises — but on measured improvements in functional capacity.
And the tool that will define this transition is the Functional Assessment Scale (FAS).
The Coming Transformation in Medical Exercise
The healthcare system is under extraordinary pressure.
Insurance reimbursement for physical rehabilitation services continues to shrink. Therapy clinics are forced to discharge individuals earlier than ever before. Yet those individuals still have significant functional limitations.
This is where medical exercise training enters the picture.
Medical Exercise Professionals are uniquely positioned to help individuals improve long-term function through structured exercise programming. But to be taken seriously by healthcare providers, exercise professionals must adopt the measurement tools used within healthcare.
Functional Assessment Scales provide exactly that.
These scales convert the abstract concept of “function” into objective, measurable data.
They allow exercise professionals to demonstrate progress in the same language used by physicians, therapists, and insurance carriers.
And that changes everything.
Functional Assessment Scales: A Snapshot of Human Function
Think of Functional Assessment Scales as a camera.
They capture a snapshot of a person's functional capability at a specific moment in time.
Through structured questions or standardized tasks, the scales evaluate multiple components of movement simultaneously, including:
- Balance
- Proprioception
- Strength
- Endurance
- Stability
- Flexibility
- Power
- Muscle fiber recruitment
- Cognitive movement control
Instead of focusing on a single joint or muscle, Functional Assessment Scales evaluate how the entire system works together to perform real-world tasks.
In other words, they measure the thing that matters most:
Can the individual function better in their daily life?
As these components improve through structured exercise programming, the score on the scale improves as well, creating a measurable indicator of progress.
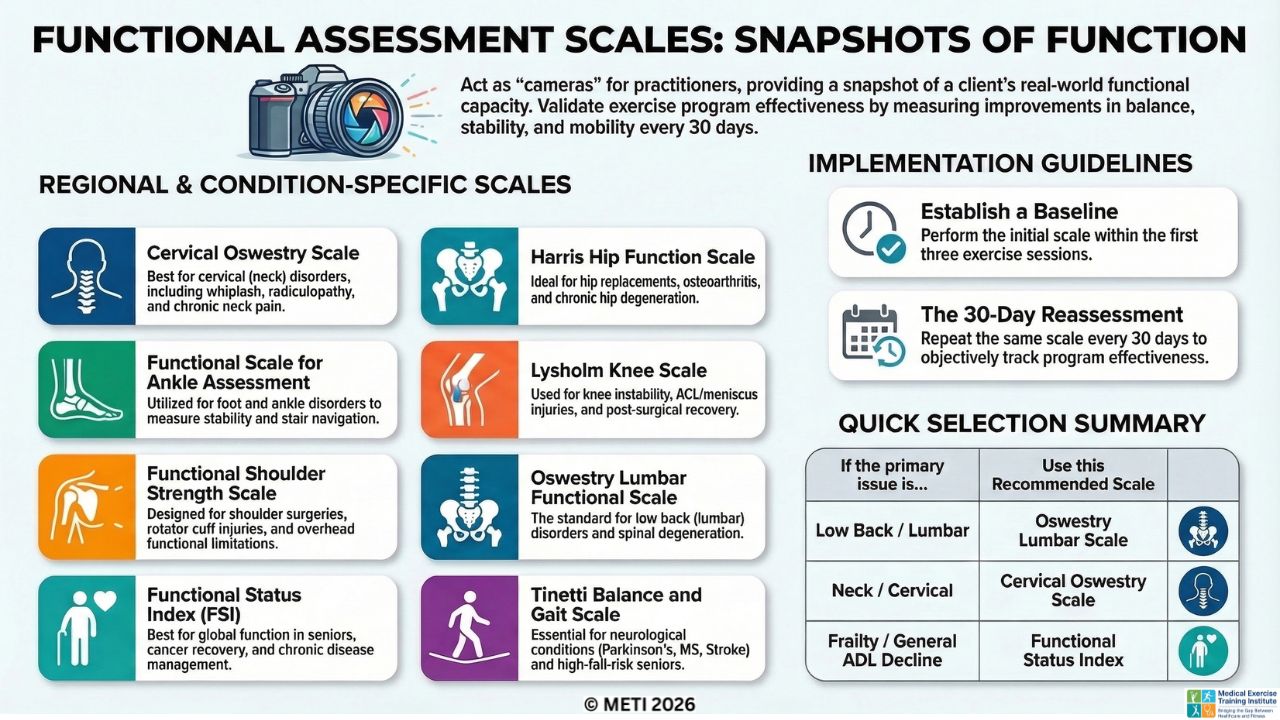
The Eight Functional Scales Every Medical Exercise Professional Should Know
Not every scale is used for every client. The scale selected should match the individual’s condition or area of dysfunction.
However, there are eight scales that every Medical Exercise Professional should understand and integrate into their assessment system.
- Tinetti Balance and Gait Scale
One of the most valuable tools for aging populations and neurological conditions.
This scale evaluates balance and walking mechanics to determine fall risk and mobility capacity.
It is especially useful for individuals with:
- Parkinson’s disease
- Stroke history
- Multiple sclerosis
- Lower extremity surgery/conditions
- Other neurological disorders
- Age-related balance deficits
The scale combines a 16-point balance score and a 12-point gait score to determine functional walking stability.
- Oswestry Lumbar Functional Scale
Developed by Gordon Waddell, this scale measures how lumbar spine disorders affect daily life.
It evaluates tasks such as:
- Sitting
- Standing
- Lifting
- Walking
- Sleeping
- Travel
Rather than simply measuring spinal mobility, it determines how back conditions influence functional independence.
- Cervical Oswestry Scale
This scale evaluates function in individuals with cervical spine disorders.
It measures how neck dysfunction influences:
- Headaches
- Reading ability
- Concentration
- Driving
- Daily work activity
- Harris Hip Function Scale
This scale is commonly used for individuals with hip conditions or hip replacement surgery.
It evaluates:
- Pain levels
- Range of motion
- Walking ability
- Stair climbing
- Daily mobility
- Lysholm Knee Scale
A valuable tool for individuals recovering from knee injuries or surgery.
The scale evaluates:
- Limping
- Swelling
- Instability
- Support requirements
- Squatting ability
- Activity tolerance
- Functional Status Index
This is an extremely valuable scale for older adults and individuals managing chronic medical conditions.
It evaluates real-world activities including:
- Personal care
- Walking
- Household chores
- Social activities
- Community mobility
- Functional Shoulder Strength Scale
This scale evaluates shoulder function in terms of:
- Range of motion
- pain
- lifting ability
- positioning capacity
- Functional Scale for Ankle Assessment
Used to evaluate function in individuals with foot or ankle disorders.
It includes functional tasks such as:
- Running
- Stair descent
- Single-leg stance
- Heel raises
- ankle stability
How Medical Exercise Professionals Should Implement Functional Scales
Using these tools effectively requires a structured system.
Step 1: Establish a Baseline
The functional scale should be administered within the first three medical exercise sessions.
This creates a baseline measurement of the client’s functional capability.
Step 2: Reassess Every 30 Days
Functional scales should be repeated every 30 days to measure improvement.
If the program is effective, the score should increase as the individual’s functional capacity improves.
Step 3: Communicate the Results
The results should be summarized and communicated to:
- the referring physician
- the physical rehabilitation provider
- the client
This creates measurable evidence that the exercise program is improving function.
Why Functional Scales Will Define the Future of the Profession
Over the next decade, the professionals who adopt Functional Assessment Scales will separate themselves from the rest of the fitness industry.
Why?
Because they will be able to prove results.
They will be able to say:
“Your client improved their functional mobility score by 32 percent in thirty days.”
That is a statement that physicians understand.
That is a statement insurance carriers understand.
And that is the statement that positions medical exercise professionals as a legitimate part of the healthcare continuum.
The Bottom Line
Random exercise does not build professional credibility.
Measured functional improvement does.
Functional Assessment Scales will soon become the bread-and-butter communication tool of Medical Exercise Professionals.
The sooner you begin integrating these tools into your practice, the sooner you begin speaking the language of healthcare.
And the professionals who speak that language will lead the future of medical exercise.
Key Takeaways for MedExPROs
- Functional outcomes are the language of healthcare.
Physicians and medical providers are not interested in isolated improvements in strength or flexibility. They want to know whether a client’s functional capacity has improved in real-world activities. - Functional Assessment Scales turn exercise into measurable evidence.
These scales convert movement performance into objective numerical scores, allowing you to demonstrate real progress and communicate effectively with healthcare providers.
Functional Assessment Scales Se…
- Measurement systems build professional credibility.
MedExPROs who consistently measure functional outcomes distinguish themselves from traditional fitness professionals by proving the value of their work through documented results.
Action Steps for MedExPROs
- Establish a baseline functional score.
Administer the appropriate Functional Assessment Scale within the first three sessions to document the client’s starting functional capacity. - Reassess every 30 days.
Repeat the same scale every month to track improvement and demonstrate measurable progress in functional performance.
Check back for our podcasts this week as we discuss more regarding functional assessment scales and their importance in growing medical exercise training.
Get Medical Exercise Training guidelines and updates!
Build your practice with tips learned over 28+ years teaching MedXPROs around the world!!
